8 Tips To Help Children With Special Needs Have Easier Medical Appointments
March 6, 2018
When caring for children with special needs in a medical setting, it is imperative to truly understand what those special needs are. This helps us to better meet the child at their level and make medical appointments as minimally traumatic as possible for them. Just because your child has special needs of some kind does not mean they are not smart or do not understand what is happening during medical appointments — they just learn and understand differently than their “typically developing” peers!
I’m a Pediatric RN, and I also have a child with special needs. My son’s name is Austin. He is 9 years old and in the third grade. Austin was diagnosed with 22q11.2 Deletion Syndrome when he was about 12 months old. Long story short, “22Q” results from a tiny portion of DNA that is missing (micro-deletion) from the 22nd chromosome. It seems to be a disorder with a wide range of severity that includes dysfunctions or anomalies in several body systems including cardiac, endocrine, immune, and GI. It is also accompanied by common physical traits and developmental delays.
I am so thankful that, while Austin has special medical, developmental, and emotional needs, they are not terribly severe. We have dealt with a fairly mild cardiac defect that has corrected itself without medical intervention of any kind as well as reflux and feeding issues that he has grown out of. However, he still struggles with hypoparathyroidism. This causes the level of calcium in his blood to decrease, causing seizures. We manage this with daily calcium supplements in the form of Tums. Austin also has many developmental and emotional needs that must be accommodated. This is where I notice the biggest need as it relates to going to the doctor, having different medical procedures, and even going to the dentist.

8 Tips To Help Children With Special Needs Have Easier Medical Appointments
While wearing my RN hat, my biggest lifelines when treating children with special needs are my patients’ parents and closest caregivers. These loved ones know what makes their kiddos tick. They know what they like, what they don’t like, and usually have a pretty good idea of how their child will respond to different situations. But let’s face it, at work, I do my job and leave the room, and the parents are left to pick up the pieces.
At home, with my Mommy hat on, I am left to pick up the pieces and put them back together after having to tell Austin he has an appointment with a doctor or the dentist. So, here are a few tips and tricks I have gathered (while wearing both hats) to help our children with special needs, as well as our typically developing children, cope with the different aspects of being a patient.
1. Determine your child’s developmental age.
This helps to know how to relate to your child and how best to explain procedures to them.
For example, most children in kindergarten are concrete and literal thinkers. Things are very black/white. When you tell your kindergartener they are going to get a shot, they easily may think they will literally be shot…like with a gun. If you tell a 13 year old they will get a shot, they probably won’t like it, but they will understand what it means and how it will affect them. However, if you tell a 13 year old who is cognitively closer to 7 years old that same information, it will be received much differently!
In my experience, it has been best to use the actual medical terms for what is going to happen; injections instead of shot, CT scan instead of “cat scan”, lab test instead of blood draw. However, I always follow it up with a simple explanation of the actual procedure using simple to understand words.
Even though Austin is 9, he has a very difficult time with abstract ideas and thought processes. I know I need to explain things to him more like I would explain them to a child who is 5 or 6 years old.
2. Do not lie to your children, no matter their age!
If your child asks, “Is it going to hurt?” when it is time for their vaccines, don’t tell them no. Be honest and try to relate it to something they understand. “It may hurt a little, like a quick pinch or bee sting. But it will be over very quickly.” Not only does this build trust between you and your little one, but it can also help combat fears and give them a reference point for what to expect.
3. Be aware of your child’s fears.
Being aware of your child’s fears simply helps you know when and how much to prepare your child for different things. If you know your son doesn’t mind going to the dentist (first, congratulations, let me know your secret), you are likely fine to let him know a few days in advance that he has a dentist appointment coming up next week. Then you can remind him maybe the evening beforehand.
However, if your kiddos are terrified of the dentist, there will be more prepping that needs to be done in order for the appointment to go more smoothly. I have to tell Austin (who is terrified of the dentist and quite apprehensive about most things relating to healthcare) about a week in advance about any medical appointment or procedure he has coming up. Then about three days prior, I like to remind him again. And then the night before his appointment, we go over exactly what the appointment is for and what he can expect.
4. Determine the best way to comfort your child.
Does your toddler have a “lovey” or other comfort object? Let them take it with them. There’s nothing wrong with making your kids as comfortable as possible during a healthcare appointment! Do they like to hold on to you? Let them. For infants, schedule their well child appointments when they will be somewhat hungry. Right after they receive their vaccinations, you can quickly put them to breast or offer a bottle for comfort.
If your 6 year old is developmentally closer to a 3 year old, allow them to still bring their favorite object. There is no shame in making a somewhat scary situation not quite so scary for your child.
5. Use comfort holds.
Comfort holds are techniques to hold your child, so they stay safe during a procedure but also have the benefit of you being there to actively support them! The Nationwide Children’s Hospital website has some excellent comfort hold suggestions I use frequently!
Chest-to-Chest Comfort Hold
The chest-to-chest hold is my favorite when Austin is getting any sort of injection. I modify it slightly since he is over 100 lbs. This would be a great way to hold your child for some vital sign checks or a blood draw from the top of the hand.
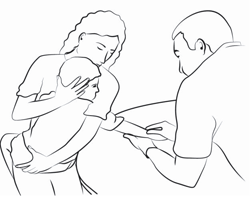
Copyright © 2015 Nationwide Children’s Hospital. All rights reserved.
Sideways Lap Sit Comfort Hold
For younger or smaller children who are still receiving injections in their legs, the sideways lap sit is an excellent hold.
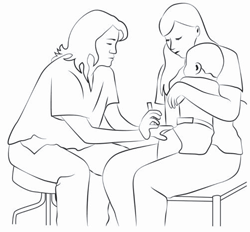
Copyright © 2015 Nationwide Children’s Hospital. All rights reserved.
Supine Comfort Hold
At work, we use the supine hold for several things including placing IV’s and inserting NG tubes.
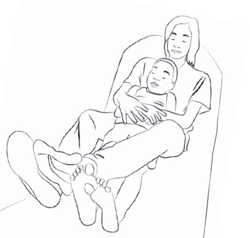
Copyright © 2015 Nationwide Children’s Hospital. All rights reserved.
Keep in mind that if your children with special needs struggle with any sort of sensory processing disorder, these holds may actually increase their anxiety. This is where knowing what frightens your child is very helpful! And as a nurse, this is where I rely heavily on my patients’ caregivers!
When doing a procedure such as nasal suctioning on an infant or even a toddler, my go-to is swaddling! When a child is swaddled tightly, they can’t use their hands to swat your hands away. The only thing they can move is their head. This can still be a difficult task, but at least you are only fighting one body part as opposed to five! Swaddling is also amazing when starting an IV. I just keep the limb that I need free out of the swaddle.
6. Use Soft Language.
Soft Language is basically the term used when you describe medical terms in a developmentally appropriate way.
For example, instead of telling my early school aged patient that I am going to insert an IV, I simply explain, “I am going to place a small straw inside your vein, so we can give your body drinks of water and medicine to help you feel better.”
I also try to find our unit’s example of what I am referring to, so the child can touch it and understand what it is.
Another common procedure is placing a NG tube. This can be explained by telling the child that I will be placing a skinny, flexible tube into their nose that goes down to their tummy and it can be used to give them medicine, fluid, or formula.
Phoenix Children’s Hospital has some amazing free apps that can help you explain different terms and procedures to your children. My favorite is an interactive app called Simply Sayin’. I use it frequently with Austin and it has definitely helped to reduce his anxiety surrounding different procedures.
7. Engage in medical play.
Medical Play is one last tool that is incredibly beneficial, especially for our children with special medical needs or those kid who are preparing for a scheduled surgery or larger procedure.
Medical play is exactly what it sounds like. It is simply allowing children to play with different medical equipment such as stethoscopes and blood pressure cuffs, so they get used to it and aren’t alarmed by those things when their health care provider uses those items during an examination.
8. Know your resources!
Most children’s hospitals have a child life department. If your child has a procedure coming up, I encourage you to reach out to your local or nearest children’s hospital and ask to speak to someone in their child life department.
A child life specialist is an expert in child development and they are an invaluable resource! They can give you tips on how to explain medical terms or procedures to your child and can point you in the right direction for the best way to prepare your child for their upcoming procedure.
Do not be afraid to be your child’s advocate!
All of the above mentioned tools and techniques are useful in the right situation. But above all, we need to know our children, regardless of their developmental level or any special needs they might have. If we are able to communicate with our children’s pediatric healthcare providers what works and does not work for our child, we will have a much better outcome during the many medical appointments that happen during childhood.
Being your child’s advocate does not just mean pressing for more testing when you know in your gut something isn’t quite right. It also means asking for a moment to help your child gather their thoughts and prepare mentally immediately before that injection they are nervous about. Advocating is requesting an appropriate comfort hold so your child tolerates a procedure better. I have upset my fair share of nurses and other support staff by requesting that they give me just a moment to position Austin in the most supportive way I can, but most of the time they are receptive and tell me they didn’t know he could be held that way!
Author Bio: Kristi DiSilvestro, Pediatric RN
Kristi DiSilvestro is a Pediatric RN, wife, and homeschooling mom to a 9-year old son with special needs and a 15 month old daughter that keeps her family laughing and on their toes at every turn! She loves helping families understand their care while in the inpatient hospital setting as well as helping them to be confident that they have all the tools and knowledge they need to take care of their little ones at home after discharge.